Shocking! Why ROM Testing Is Better Than Most Shoulder Tests
Posted By: Andy Barker
It teaches you enough to be ‘safe’ and diagnose simple injuries.
But guess what?
Most injuries aren’t quite as simple or clear cut as you were told.
The classic textbook shoulder, knee or lower back pain patient never walks in to your clinic.
In fact, I don’t even think these patients exist!
Patients always have other issues…
They have previous injures that complicate your assessment…
Or present with symptoms that do NOT fit that textbook clinical pattern.
As a New Grad you lack experience treating injuries, like the shoulder, and when things do not go well, you feel out of your depth.
When your objective tests don’t match your subjective question’s, it throws you sideways and you start to doubt yourself.
You doubt your own competency and this leads to an increasing lack confidence in your abilities as a therapist.
You worry that you might not be good enough.
You worry what sort of patient will walk through the door next…
And you question whether or not you will have the skills to work out what their problem is.
If you have already qualified you will know exactly what I am talking about.
If you are still studying you have all this to come!
But there is another way to make sense of your patient assessments and it’s not some magic test or assessment method.
It’s actually much simpler than that.
Lets take a look…
You Know More Than You Think
I have know doubt some of the stuff you are already doing with your patients is great.
Think of all that time you spent at Uni and on placements learning and the knowledge you already have.
You have the skills and enough knowledge to get started.
When I first start working with any New Grad the first thing I try to attain is what they are struggling with the most…
So we can get right to work to fix that up asap.
That might be a problem with the subjective assessment, or knowing how to confidently progress and regress a patients rehab or a therapist having difficulty getting their foot in the door in a clinic or sports club.
Additionally, I want to know what they are good at.
Sometimes we lose sight of our main attributes and the things we are good at…
Choosing to focus entirely on improving our weaknesses.
But, why not improve your weakness and also further improve and maximise your strengths?
Maybe you are more confident with rehab than you are with your assessments.
Maybe its the other way around.
The point here is that you do have the skills to help your patients…
You just need to be able to apply the skills and knowledge you learnt at Uni in the real world.
The first step to do this is to ask yourself why…
Ask Yourself WHY
The biggest thing is understanding WHY you are doing something.
Whether it is a question as part of your subjective assessment…
A particular special test…
Or an exercise you prescribe a patient as part of their home exercise programme…
Do NOT just doing something of the sake of it…
Or just because that was how you were taught to do it at Uni…
Or do it because that is how you’ve always done it.
Ask yourself why you are are asking that question, using that test or prescribing that specific exercise.
Can you reason why and provide a rationale?
Think about the last patient you saw that you got stuck with.
What part of their assessment threw you out?
Did you get the information you needed to make the right diagnosis?
Was the treatment technique or exercise you picked the right one i.e. was it chosen to fix one of the patients identified problems or…
Did you just release their pectorals or prescribe a posterior rotator cuff exercise because they had anterior shoulder pain?
This is basic but this is clinical reasoning.
It is spoken about so much during your Uni training…
Yet no one actually applies it in real life with real patients.
Then you wonder why you can’t get the diagnosis right, or you choose the wrong treatment technique or rehab exercise with your patient and it doesn’t work.
Here’s how to make clinically reasoning easier…
Know The Evidence Base & Keep It Simple
To help you clinically reason what you are doing, you need to know the evidence base.
Relating this to the shoulder…
It is well evidenced that many special tests have poor diagnostic accuracy.
In short, most have poor sensitivity and specificity and many can’t differentiate between different pathologies making it very difficult for you to make a confident diagnosis.
But knowing the evidence base and keeping it simple can actually be very helpful…
Regardless of whether the special tests at the shoulder are any good or not.
Here’s what I mean…
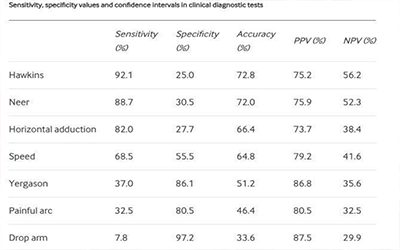
Just testing your patients ROM and observing a ‘painful arc’ is more specific (by a long way) to diagnose shoulder ‘impingement’ than commonly used impingement tests like Speed’s test, Neer’s test and even the Hawkins-Kennedy test!
So if you suspect your patient has shoulder impingement then why would you use these ‘special’ tests when they are not even as good as a simple ROM test?
If you think about it logically it makes no sense.
If you do a good job with your subjective and your basic objective assessment, including range of movement testing, your observation and palpation and output (strength) testing…
Do you even need to use special tests?
Often you will find you don’t.
Don’t just do a test because that is what you think you should do.
Ask yourself…
What information will this test give me?
Is it going to add any useful information to help me make a diagnosis or help me to decide the next step for my patient?
If you think it might help, do the test.
If you don’t think it will help, then don’t do the test.
Save your time and effort and get going with your treatments and rehab.
This sounds super simple…
Because it is.
Near every New Grad I speak to is overcomplicating their assessments, treatments and rehab.
Looking for some magic special test, or technique or rehab exercise they’ve seen on Instagram…
That will fix all their patients problems.
I bet you have done the same…
Jumping from test to test…
Trying every treatment technique or different rehab exercises when your patient does not progress as you think they should…
Probably without a second thought as to WHY you are doing that test, technique or prescribing that exercise.
You feel under pressure as your patient is not improving…
So you try anything and cross your fingers…
Hoping that something will work…
Without actually thinking and reasoning what might actually work.
Making sense of the shoulder (and all your patient assessments)
I know the shoulder can feel daunting and so many therapists struggle with this joint.
This is why I put together this FREE resource…
In this special resource you will also discover…
1) The #1 Reason Why New Grads Can’t Seem To Get The Right Diagnosis No Matter How Hard They Try!
2) Why You Should Never Trust People Who Tell You That The Shoulder Is ‘Complex’ And What You Should Do Instead
3) The Honest Truth About Getting Great Results With Shoulder Pain Patients And Why It Can Be So Much Easier Than You Ever Imagined!
And Much, Much More!
PS. Even though this is a ‘shoulder’ resource, all the content and what you can learn can be applied to ALL your other joint assessments, treatments and rehab!
Get Your FREE COPY Right HERE.
Enjoy!
Andy